
Understanding Your Hormonal Rhythm: How the Menstrual Cycle Works and When to Get Help
Introduction
Every month, a woman’s body goes through a complex yet beautifully balanced process — the menstrual cycle.
While many associate it only with menstruation, it’s actually a sequence of hormonal changes that affect not just reproduction, but overall health.
Understanding how these hormones work helps women recognize what’s normal, what’s not, and when to seek help.
1. The Basics of the Menstrual Cycle
The menstrual cycle has two main components: the ovarian cycle and the uterine (endometrial) cycle.
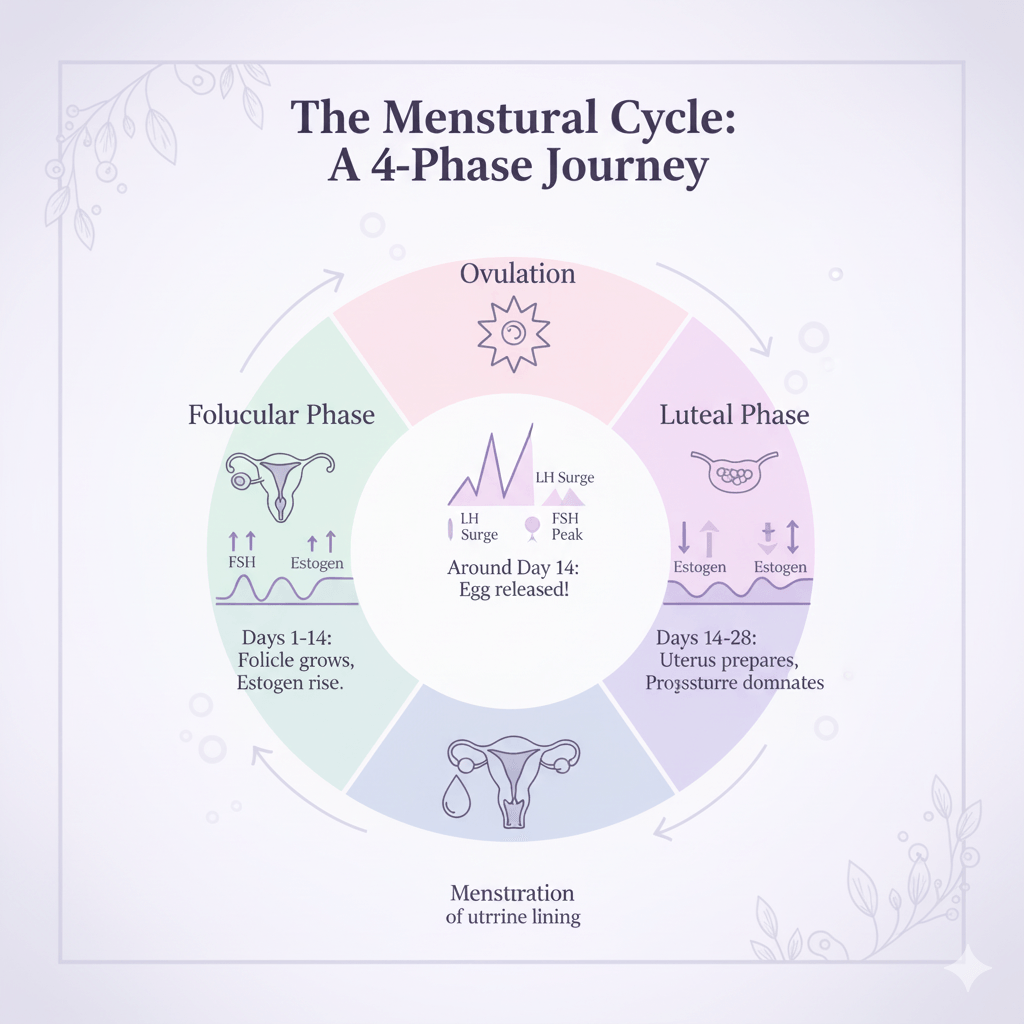
Follicular phase (Day 1–14):
It begins on the first day of bleeding.
The pituitary gland releases Follicle-Stimulating Hormone (FSH), prompting an ovarian follicle to mature and produce estrogen.
Ovulation (Around Day 14):
A surge in Luteinizing Hormone (LH) causes the release of an egg from the ovary.
Luteal phase (Day 15–28):
After ovulation, the empty follicle turns into the corpus luteum, producing progesterone to prepare the uterine lining for pregnancy.
Menstruation:
If fertilization doesn’t occur, progesterone drops, the uterine lining sheds, and a new cycle begins.
A healthy menstrual cycle typically lasts 21–35 days, with bleeding for 2–7 days.
Experts now consider the menstrual cycle a “fifth vital sign” of women’s health because it reflects hormonal and metabolic balance.
2. The Key Hormones Involved
The menstrual cycle is regulated by precise communication between the brain, pituitary gland, and ovaries.
Gonadotropin-Releasing Hormone (GnRH):
Released by the hypothalamus, it controls FSH and LH secretion.
FSH & LH: These pituitary hormones stimulate follicle growth and trigger ovulation.
Estrogen: Thickens the uterine lining and prepares the body for ovulation.
Progesterone: Prepares and stabilizes the uterine lining after ovulation.
Other hormones: Thyroid hormones, prolactin, insulin, and adrenal hormones also influence menstrual health. (Facts About Fertility)
When these hormones stay in balance, cycles are predictable and healthy.
But if one pathway is disrupted, the entire rhythm can shift.
3. What Causes Irregular Cycles?
Cycle irregularities are common and often linked to hormonal imbalance or lifestyle factors.
The most frequent causes include:
Polycystic Ovary Syndrome (PCOS): High androgen levels and abnormal LH/FSH ratios interfere with ovulation.
Thyroid disorders: Hypothyroidism often causes heavy, prolonged bleeding; hyperthyroidism may shorten or lighten periods.
Elevated prolactin levels: Suppresses GnRH and prevents ovulation.
Lifestyle factors: Extreme dieting, rapid weight loss, obesity, or excessive exercise disturb the hormonal axis.
Stress: Physical or emotional stress alters hormone release patterns.
Warning signs that need medical evaluation:
Cycles shorter than 21 days or longer than 35 days
Bleeding heavier than usual or lasting more than 7 days
Absence of periods for 3–6 months (not due to pregnancy)
Spotting between periods or after intercourse
Sudden, unexplained changes in your usual cycle pattern
Irregular cycles can indicate deeper endocrine problems and may increase long-term risks such as infertility, insulin resistance, or cardiovascular disease.
4. Why It Matters Beyond Reproduction
Your menstrual cycle isn’t only about fertility — it affects multiple aspects of health.
Bone Health: Low estrogen reduces bone mineral density, raising osteoporosis risk.
Heart Health: Irregular cycles have been linked with a higher risk of metabolic syndrome and type 2 diabetes.
Emotional Well-Being: Hormonal fluctuations influence mood and sleep patterns.
Quality of Life: Painful or unpredictable periods can cause fatigue, anxiety, and social discomfort.
Recognizing these links encourages early evaluation and management to prevent complications later in life.
5. How to Support a Healthy Cycle
1. Track your cycle:
Record your period start dates, duration, and any symptoms. Apps or paper trackers help identify patterns.
2. Maintain a healthy weight:
Both underweight and obesity can suppress normal hormone signaling.
3. Eat a balanced diet:
Include iron, vitamin D, calcium, and omega-3 fatty acids to support hormonal and bone health.
4. Manage stress:
Techniques like meditation, deep breathing, or yoga can normalize hormonal rhythms.
5. Exercise moderately:
Aim for consistent, moderate physical activity rather than extremes.
6. Get enough sleep:
Poor sleep affects cortisol and reproductive hormone levels.
7. Regular check-ups:
If you experience significant changes, consult your healthcare provider.
They may recommend hormone testing (TSH, prolactin, LH, FSH) or ultrasound imaging for diagnosis.
Conclusion
The menstrual cycle is more than just a monthly routine—it’s a reflection of your body’s internal harmony.
Understanding the hormonal rhythm behind it allows you to take control of your health, notice early warning signs, and make informed choices about lifestyle and care.
When something feels off, never ignore it—your period can reveal more about your well-being than you might think.
